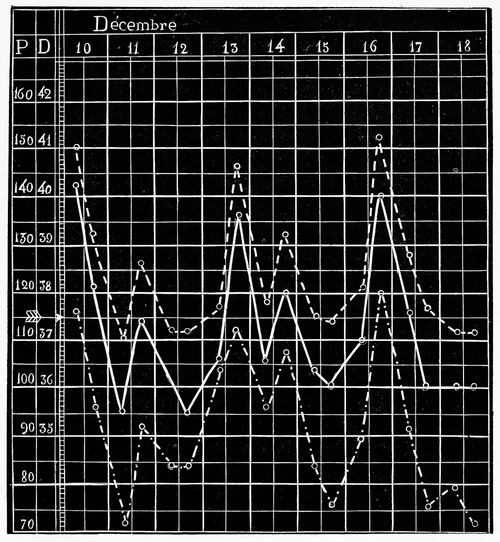
Physicians have long been interested in body temperature and physiologists occasionally measure it for research purposes. Systematic measurements, however, did not become established in the new hospitals until the 19th century. This is how doctors translate a subjectively perceived condition into a number. At first, it remained open as to what exactly the measured values meant. The breakthrough as a standard diagnostic method was helped by the representation in curves. They made it possible to identify typical fever courses of individual diseases. Shortly before 1900, taking a temperature reached private households and advice literature, thereby becoming commonplace.
From research instrument to everyday object
The first thermometers were long and unwieldy and were mainly used in research. In the 19th century, a 15-centimetre-long thermometer was introduced that worked by expanding a column of mercury. Form and function remained almost unchanged for a long time. In the 20th century, electrical, then digital and finally infrared thermometers appeared. They measured accurately and, especially with the latter, within a few seconds. However, the portable pocket thermometer based on toxic mercury persisted and was used until the 1990s.
Fever without measuring
Today, a fever is considered to be an elevated body temperature. With the systematic measurements of the 19th century, a limit value of 37.5 degrees Celsius was established for elevated temperature. In the 18th century, doctors did not record the temperature with numbers. Albrecht von Haller, for example, in the context of an epidemic "catarrhal fever" in 1733, states: "At night I fevered violently and reached a heat that was not at all moderate". In retrospect, it is not possible to say how high this fever was, nor to determine what Haller understood by "moderate" heat.